Designing Better Healthcare Experiences
The Center for Health Design, UW Health + Steelcase Health share ways healthcare spaces can support today's needs.
We know the space around us can have a profound impact on health outcomes — influencing the overall wellbeing of everyone involved in the complex work of care. It’s within these settings that people go through a wide range of experiences and emotions. Think about sitting in a waiting room, awaiting the outcome of a procedure for your loved one, or the anxiety of making decisions about your own healthcare – not to mention the care providers who are on an emotional journey with their patients.
Recently, Steelcase hosted a Work Better webinar (watch on demand now) to discuss the trends driving healthcare design and how that can lead to better care experiences for patients, their families, clinicians and staff.
Participants:
Michael McKay, Director of planning, design and construction, UW Health – Madison
Ellen Taylor, vice president for research, The Center for Health Design
Seth Starner, advanced explorations, Steelcase Health
Host: Katie Pace, Work Better communications director, Steelcase
Katie Pace: Let’s start by asking each of you the same question. What is the biggest challenge organizations are facing with their healthcare spaces as we move beyond the pandemic?
Michael McKay: Well, for us at UW Health, it’s space and the lack thereof, the management and use of that space is one of the most critical factors we deal with every day.
Ellen Taylor: In talking to a lot of organizations, I find everybody is concerned about the financial side of things. Healthcare organizations are facing the squeeze everybody is feeling, and there are a lot of questions about the future of capital and what types of projects can actually be accomplished.
Seth Starner: Building on what Ellen said – it’s clinician retention and finding and paying for the staff that hospitals need to provide care. And that is getting to be harder and harder, especially post Covid.
KP: When we talk about the current evolution of healthcare spaces – we hear the word “hospitality.” Most people think of a ‘hotel’ but that’s not quite it. What does the term ‘hospitality’ mean to you in the context of healthcare spaces?
MM: We have always focused on the patient and being patient-centered, but these days we also have to focus on being more staff-centered, and experience focused with an intentionality around design. It also relates to care and attention – the basics of hospitality, and how we deliver that patient experience in the spaces that our patients and families are coming to for care. So it’s about the experience.
From a facility perspective, hospitality equals brand for us. We know that the space for healthcare can impact one’s perception of the level of care, as well as the overall experience. That’s the tallest order for us on the facility side. “Healthcare” is making sure that our facilities deliver on the remarkable level of healthcare for which UW Health is known.


KP: Ellen, you have a slightly different take.
ET: I think there are two sides to this. From a hospitality perspective, we don’t want the traditional institutional type of aesthetic – the old hospital room that’s just all white, with no amenities and no design features, with poor access to daylight and views. But the flip side is, it is still a hospital. It’s not the same thing as a hotel or a restaurant where you’re choosing to go. You have to be here, and the circumstances are different. In a hotel, for example, you’re not expecting somebody to come uninvited into your room and see what you’re doing or how you’re doing. It can be a little bit of a frustration for nurses who understand they have to take care of this person, and also feel like they’re somehow invading a space that’s been created with a family zone and lots of people visiting.
There was a project we worked on several years ago – a children’s hospital. It was an incredibly beautiful design, and they moved from this older facility where everybody was piled on top of each other. They didn’t have any space for families to visit. Certainly, no overnight space. When they moved into the new facility everybody was so appreciative that the parents could come and stay and bring the rest of the family, and everybody could be part of this very supportive environment for the child. That’s wonderful. Except, they would then also do things like bring blankets from home and hang them over the windows, so that the light from the hallway didn’t disturb them at night. Yet the nurses need access to be able to see what’s going on in the room. So again, it’s this balance. It’s a difficult balance to figure out what we need to do to make patients comfortable, and ultimately help them heal faster, but also provide care effectively from the provider side.
KP: Seth, you talk about this notion of hospitality from a clinical point of view – can you elaborate?
SS: When you’re there, it is typically an emotionally fraught time. You’re not there for fun. It’s not a pleasurable experience. You’re there because you have a big need. In the past, hospital spaces were very clinical, and that was meant to both convey and provide physical safety.
Hospitality and this whole idea of a hotel-like vibe – what’s really happening there is a desire to provide emotional safety. For clinicians, they forget about the space because they go to work there every day. For the rest of us who don’t work in healthcare on a normal basis, however, it’s an odd space. So, I think hospitality is trying to create a more normative experience to help people feel like it is like other places they’ve been. They may be here for different reasons, but they’re comfortable. They’re safe. They’re becoming calmer, or confident. There are all these emotions that we’re trying to manage for these individuals when they’re coming into this space.
From a furniture standpoint. I’m always thinking about how you create a delightfully aesthetic piece of furniture yet meet all those clinical needs: easy to clean, can be cleaned repeatedly with some pretty caustic solutions, and survive that 24-7 use. The whole environment needs to be kind of hardened to take that abuse and still look good and meet all those physical and emotional safety queues.

Also, most of the time at a clinic, you’re waiting. So how can we help create more productive waiting. For instance, can we give someone a place to charge their phone or work on a computer? It’s about creating a diversity of environments, so other parts of life can continue while you’re engaged in this experience. If you’re stressed, it’s hard to hear and to comprehend important medical discussions with your doctor. So, whatever we can do to take the stress level down a notch, so that therapeutic clinical interaction can happen in a better way, that’s the priority.
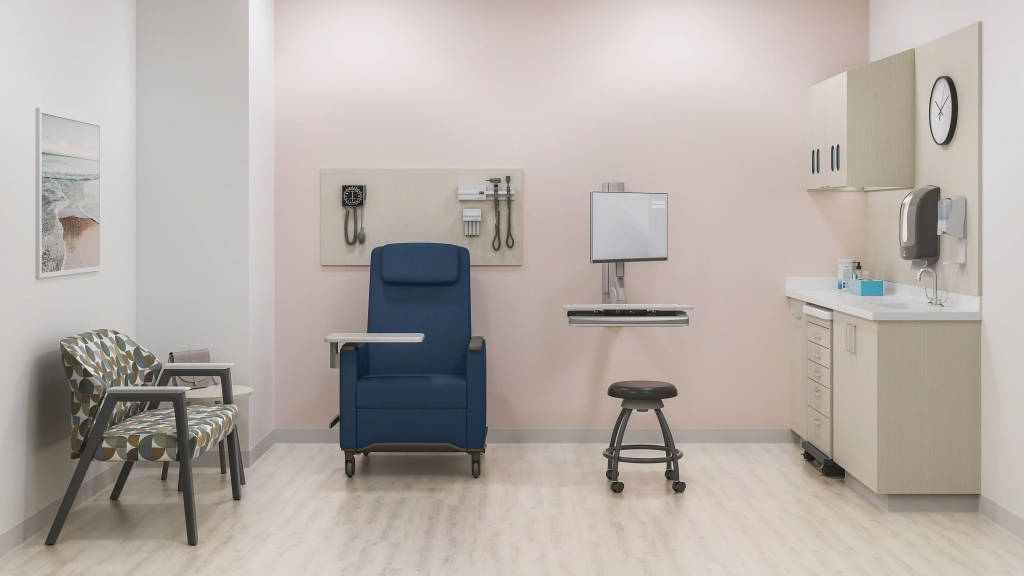

MM: Just to add to that, we are seeing that our providers want that patient-family experience in our patient and exam rooms. We are adding more soft seating because we realize patients rely on their family for care, and it’s good to have the family as care providers in the room with the patient. It’s especially helpful when family members are hearing the interaction with the provider so they can understand what’s going on and understand what they’re going to need to do to support their loved one through their care once they get home.
KP: How big of a problem is clinician burnout. And how can space help?
ET: I think this is huge, and it’s important to talk about some of the cultural aspects. The built environment should certainly support some of these issues to relieve some of the stress and anxiety, but it can’t, by itself, be the only solution. We’ve always talked about the impact of space on staff. I think COVID really brought this to the forefront even more. I do have a concern that, as we start to head back into a greater sense of normalcy, this will start to fall off the radar. But certainly, everybody is facing some stress associated with people leaving the profession. We need to do more to keep people, and if that means providing space to support them, that’s something that needs to be on our radar. It’s everything from efficient layout configuration, so that people can do their job better and not feel like they’re wasting time, running back and forth to supply rooms, but also providing respite and break space. Layout is very important in that regard. Doctors and nurses feel an obligation to be near their patients. If the break room is a 10-minute walk away from the unit, they’re not going to leave. Really developing that organizational culture that supports the fact that you should take a break for your own mental health and wellbeing but then also provide the physical space that reinforces that. It’s a systems approach, but incredibly important.
KP: Michael, you’ve been part of launching some projects, how are you thinking about taking care of the caretakers?
MM: It is important and frankly in the past we haven’t allocated enough space for our staff – that ‘off stage’ space that’s on or near the units. So, it has changed, and it’s impacted our planning moving forward.

Taking this type of approach with outdoor spaces is terribly important to us, and we’re looking at our existing facilities where we are in the process of converting several of the rooftops into winter gardens and outdoor spaces that staff pass through on the way in and out of work. These are areas where staff can have a break coming into work to get mentally prepared, and then, when they’re leaving, if they just need some downtime or a place to go and be in private and decompress from the day that they just had.

We also have indoor clinician collaboration zones where providers and clinicians can get away and be in their own space – let their emotions out, if need be, and decompress from some stressful event they might have experienced. One space has an aqua fireplace – it’s water vapor emulating flames. It will be a place of warmth – we’re bringing in some of those basic elements that are critical and missing sometimes from our design. It’s feeding into that notion of hospitality but directed to our staff.

KP: Another aspect of healthcare that has changed dramatically is the rise in the need for behavioral health treatment. Seth, we know you’ve done a lot of work understanding this emerging need – can you tell us more about what behavioral health includes and how things have changed from before the pandemic?
SS: Behavioral health has been an issue. Pre-COVID there was already a shortage of treatment. It was hard to get appointments. I think the stigma around behavioral health has come down. I’m not going to say it’s gone, but I think people recognize that it is something that needs to be treated like you would a physical ailment. COVID exacerbated the problem – speaking for everyone who lived through those three years, you know it – it was not an easy time. I think for many people, it stretched their capabilities to deal with it. We’ve seen a huge increase, especially in children, but also in adults. So, we need special spaces for that. Hospital systems and everyone who’s involved in that space is trying to figure out how we offer treatment in a way that doesn’t create stigma. Again, trying to create a normative experience, while even having a little stricter physical safety requirements around self-harm. The furniture especially needs to make sure that it cannot be used in any way that would be detrimental to the patient or to those around them. Again, that tension between making it feel calming and warm and welcoming while still being very safe – finding that balance between emotional safety and physical safety is a challenge, and one that we’re working on vigorously.
KP: To that end, Ellen, how do you see that challenge playing out in design? And are there any interesting solutions that you’ve seen?
ET: It used to be that we would talk about behavioral and mental health with respect to secure psychiatric units. We would have all these issues associated with involuntary behavior and admission into these types of units, and it was about trying to protect the patients and trying to protect the staff that work with them. But now, we’re increasingly more understanding, and perhaps a little bit more empathetic that somebody can have a mental and behavioral health issue without being in a secure psychiatric unit. Certainly, we still need to be concerned about safety in those types of facilities. However, I think there needs to be a more holistic understanding of what we face everywhere. I was looking at a research study recently, and they found, through a retrospective review of data, that half of the patients that were admitted to the hospital over a period were found to have a mental behavioral health issue. So, there is this idea of comorbidity, and that people may be seeking healthcare but also have an underlying mental and behavioral health issue. Statistically that means the person has a greater chance of experiencing a worse outcome.
Increasingly, there is starting to be at least discussion around how you design these traditional healthcare spaces with safety in mind for a mental behavioral health contingent that may be in your facility. Getting back to the hospitality question. We certainly want these to be healing environments. But how do we balance that healing and safety perspective? There’s a place to think about this differently, and to make our facilities a little bit more accommodating for this, and as we’re moving past the stigma, I think that will be an easier conversation to have.
Take a Tour
We invite you to take the next step toward creating your ideal healthcare spaces and experiences. Connect with us to schedule an expert-guided virtual tour of our newest spaces for healthcare from waiting spaces to patient rooms, and everything in between.


